Self Management after a Neurological Injury
Amy Bean
Wednesday, April 1st, 2020
Self Management after a stroke, head injury or other neurological injury can be interpreted differently depending on whether you are the person who has suffered the injury, therapist or family member/carer. In this piece we try to explain what the principles are, how it should be done and what the evidence is behind it…
So what actually is Self Management?
In a study completed in 2017 by the Stroke Association (Stroke Association 2017) which looked at how both therapists and stroke survivors interpret it, they found that therapists view Self Management as the process in which individuals take an active role in their rehab and a responsibility to manage their own recovery following their stroke.
In the wake of the outbreak and spread of Coronavirus, this is now more important than it has ever been. In the case for many people it is now not so much of a choice but a necessity. There is a growing adoption of the use of video where face to face are no longer possible in addition to telephone support and advice and education can still be provided effectively this way.
The instigators of self management are usually health professionals, such as your Physiotherapist, Occupational Therapist or Speech and Language Therapist. However it could be yourself or your family/friends or carers.
The ultimate goal will be the same whoever is the driver and this is to improve the quality of life and self-efficacy.
What is the process and how does it work?
During therapy, advice and education on problem solving, decision-making and goal setting are provided within the context of rehab. This might be to the person themselves, and/or a family member or carer.
Ideally the earlier this happens after the neurological injury the better, as this has been shown to give better results in the ability to perform every day activities in the long term (Parke et al, 2015).
By going through this education process, this will form a patient/healthcare provider partnership resulting in the ability to find and utilise resources for ongoing rehabilitation. These resources may be online such as exercise videos, “how to” advice or information on relevant community services such as Stroke clubs, Gyms, and carer support groups. Our own Saebo UK YouTube Channel has a growing resource of tips and exercise ideas for use with our Saebo products; and M.O.T.O.R is great channel for online exercises
In the earlier stages of rehab within the hospital setting, self management may focus on basic function related goals e.g. to be able to wash and dress independently or sit to stand. This may involve showing you how to break down the task, work on the separate components and then how to progress each separate component to work towards being able to complete the task as a whole.
Later stages of this, predominantly with an Occupational Therapist, might be focused on re integration back into the community and medical management such as secondary disease prevention.
Examples might be providing advice on a staggered return to work, being able to go to the shops, or even just being able to get in and out of a car safely. There may be also be education around fatigue management if appropriate. What is looked at should be focused on the person’s own goals and needs.
For secondary disease prevention it may be education around risk factors such as diet, exercise and medication. The NHS Live Well section on their website has a lot of useful pages around this as a starting point
The table below borrowed from Parke et al (2015) provides a useful summary of the process:
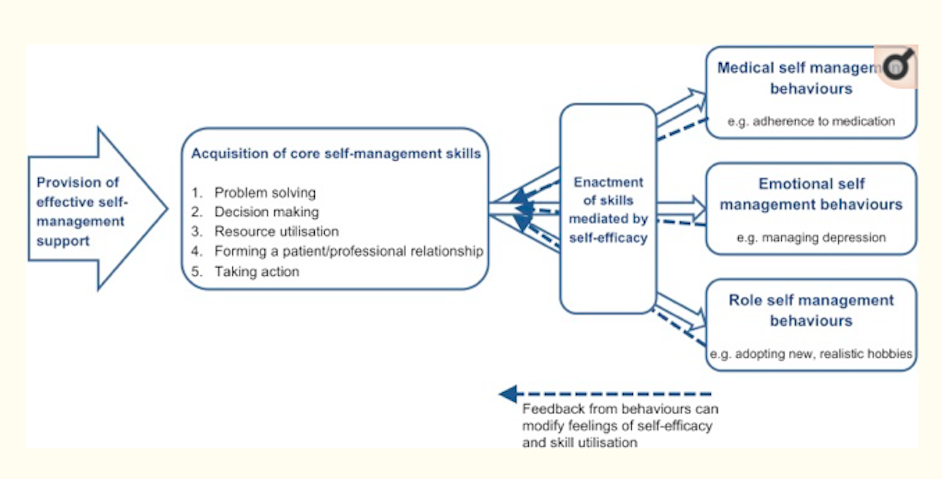
Is there good evidence to support this approach?
Yes! In the 2016 UK National Stroke Guidelines it is recommended that stroke survivors, where appropriate, should receive training to provide them with the necessary skills in being able to self manage their rehab. In addition to this, therapists need to have received training to action this and be able to work in a system that supports this.
Evidence to support self management in more chronic, long term conditions is well established and is much more routine than stroke. However, this is changing with more recent research. A leading voice in the UK for further research in the field of this is Fiona Jones
Misconceptions of Self Management
Self management is not a “just do it yourself” approach where the person is expected to do their own rehab due to lack of resources or because they are perceived to be able to manage on their own.
It should also be more than just the handing out of disease specific self help leaflets or sign posting to websites.
Where possible and appropriate, advice and guidance on self management skills should be a discussion to have with your therapist if it has not already been instigated.
Technology to assist
At Saebo we are supporters of self management. The rehab journey can be long and hard for many and with the right skills and  education at the start of the journey this can only help the outcome. The appropriate piece of technology can provide a helping hand, such our SaeboStim Pro electrical stimulation device helping open the coffee jar using the trigger button. We are always on hand to help advice with how to maximise use to help towards your own goals.
education at the start of the journey this can only help the outcome. The appropriate piece of technology can provide a helping hand, such our SaeboStim Pro electrical stimulation device helping open the coffee jar using the trigger button. We are always on hand to help advice with how to maximise use to help towards your own goals.
If you are not sure which Saebo product may be suitable, our Clinical Team are here to help and advise


